Start off my day with an Indian lady with necrotising fascitis of the lower limb for wound debridement.. She started crying since entering the OT.. She said she is scared but don't know scared of what... I explained to her about spinal anaesthesia but she started crying again & refused any surgery or further intervention. Well, I can give her General Anaesthesia(GA) but the problem is she has so many loose teeth.. all her incisors & canine teeth are loose. Very shaky indeed.. Can be pulled out easily without any force. I really have no idea how she eat with such loose teeth & why she keeps all those loose teeth? I guess she is scared to go for teeth extraction as well.. Risk of accidental tooth extraction (& more scary thin is tooth aspiration to the bronchus) if giving GA. After reassurance & wasting so much saliva talking to her, then she finally agreed to continue on with the operation.. I sedated her with iv midazolam and iv ketamine prior to spinal anaesthesia. Post operatively, she was smiling.. Well, nothing scary, right? :)
I have quite a number of orthopaedic cases yesterday.. Followed by open fracture right metacarpal for wound debridement, open reduction & mini plate. This girl has receeding chin but thank God, no difficult intubation :) Cormack & Lehane 2 with cricoid pressure..
I proceed with Wound Debridement & Split Skin Graft(or SSG) after that for a 77 years old lady... When the patient arrived to OT; I flipped through the old GA forms & I found out that... patient just underwent surgery two weeks ago, & apparently she has Parkinson Disease with stiff neck & very limited neck movement. She was intubated with awake fiberoptic intubation previously & post intubation, assessment with laryngoscopy showed Cormack & Lehane 3 vocal cord !!! Mmmm... next time, might be I really shouldn't do any SSG cases on weekends already.. Since this is non urgent case. I taste bagging with face mask & able to maintain airway.. before I give any drugs. So I just insert in Laryngeal Mask Airway (LMA) for her. The insertion of LMA is easy but have problems trying to secure it, cos the patient doesn't have any teeth at all, & the LMA keep on sliding to the side of the mouth.. I changed to size 4 LMA but the same problem occured as well.. Well, but manage to seal the airway properly, just that the position of the LMA is a bit weird..
The next case I did was tracheostomy. This patient has craniotomy & evacuation of hematoma few days ago.. GCS about 7/15 with poor gag & cough reflex..
After that, I did another 79 years old lady (so many geriatric patients today) for Incision & Drainage (I&D) for extensive left upper limb abscess & cellulitis.
Followed by another cases of Left knee abscess & I was told by the HO who booked the case that patient is for I & D only. I asked the HO specifically whether are they doing any extra procedures or not like removing the implant etc.. And the answer given was "no..." This lady has bilateral total knee replacement done earlier on for osteo arthritis both knees but complicated with infected implant. The TKR implant was removed earlier on & the space was filled up with cemented material, but she still have recurrent abscess..
This lady has very difficult venous access & really have hard time looking for veins.. I manage to secure a 20 gauge branula over the left hand (Well, since it's I & D, i didn't anticipate any much problem or bleeding or whatsoever.. She has nice neck vein actually, but that's my last resort if I unable to get any peripheral lines on the upper limbs) On table only, I noticed they actually want to do more than just mere I & D. Removing the cemented implant..& External Fixator if the wound is dirty or fusing the knee if the wound is clean.. Patient bleed so much intra operatively, more than 1.5 liter & her blood pressure was very labile, I gave her many boluses of iv ephedrine & iv phenylephrine to maintain the blood pressure while running fast colloid & blood products. She looked so pale.. I wanted to set some more big lines on the neck, but now, the neck veins collapsed already after the bleeding episodes.. became non visible already.. After the surgeon finish stitching the wound, I quickly set an 16 G angiocath at the right femoral vein & continue on running fluid for her. Her hemodynamic status stabilised after transfusing second pint of blood... These surgeons ah.. Inform earlier on lah what they want to do .. :(
The excitement haven't stop yet.. So many orthopaedic cases. Have another young boy. Allerged MVA with open fracture of ulna for wound debridement & open reduction internal fixation (ORIF). Then I had a guy fell down from height and had a penetrating injury to the neck with profuse bleeding. Blood is splurting out from the neck.. For exploration, ? vessel injury.. He had few puncture wound & laceration at the upper limbs & lower limbs as well.. Very tachycardic on arrival to A&E with heart rate of 150+. Manage to stabilise blood pressure & heart rate after fluid resuscitation but patient was pale due to bleeding.. Blood transfusion started intra op, Luckily it's just external jugular vein injury & manage to secure the bleeder fast :) The orthopaedic team did the toilet & suturin (T&S) for the laceration wound.. At this time, it's past 12 midnight already..
I have another case after that, middle age thin guy who swallowed his denture during drinking.. aiyoh.. From XRay, the level is at T1).. The ENT team did the oesophagoscopy & removal of denture.. Procedure was quite fast & patient was extubated half an hour later on.. It's 1:30 am already by then..
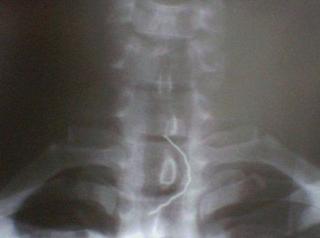
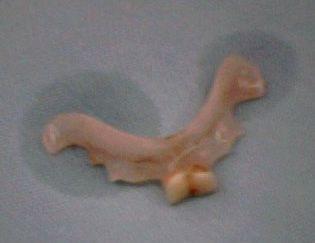
Post extubation.. noted patient having noisy breathing and unable to talk.. Saturation well maintained initially at 99% to 100% on ventimask 60% oxygen. He was prop up. Secretions ++ but he unable to cough out. He had difficulty in breathing with SOB. Impression was ? laryngospasm with upper airway obstruction. iv dexamethasone 8 mg given & patient was prop up almost 90 degree.. Nebuliser given.. Saturation was around 90 to 96%. Lungs clear.. Emergency intubation trolley was standby. Conditions much improved after neb & resolved.. maintaing SpO2 985 to 100%. He was observed for one hour plus in the recovery bay before sending him back to the ward at 3 am..(to be nursed in acute cubicle with oxygen supplement overnight & pulse oxymeter monitoring). What a day.. Finally can go to rest at 3 am in the early morning..
11 comments:
Gasman,
haha.. yeah, guess that occurs everywhere :) Even in the previous hospital where I worked before as well
wot the ...?? dentures also can swallow?? *shock*
Goodness!!! How on earth???
Anyway, loktor, you've tagged http://babeinthecitykl.blogspot.com/2005/06/meme-cook-next-door.html hehehe have fun
D notti,
In fact, this is not the first time people swallowing dentures leh.. Have seen it several times already :)
Gasman,
err? another case of bottle up in the ass? We have a similar case over here in our ICU as well... Wonder, is it the same patient u are talking about as well? :D
If I didn't remember wrongly, that patient is a Mat Salleh... but this incident occured quite long time ago already..
BabeKL,
hahahha... I have read what u write over there already :P I do cook other things as well lah, besides instant noodle, kekekeke ......
btw, Do I have to answer all those questions back ah ? Okie okie.. will try to do so one of these days :P
bottles wedged up "there"? xx( yuck
:O
my God ..!! what a busy day!
What's up Doc, Have you seen jack Ass The Moive ? Hope no one pulls a prank like that at your hospital.
btw "after dat you get 3 other people to do the same "....! Don't send it over.. :)
Fred,
that on still consider okie loh.. I have go through worse on call than this.. like staying up awake & work non stop for more than 24 hours.. or things like takin dinner at 12 midnight etc...
Cookengr,
Haven't see jack Ass the Movie yet :)
Keep fingers crossed loh, heheh..
Aiyoh.. why u mentioned it so fast, or else sure I will send over to u :P
Post a Comment